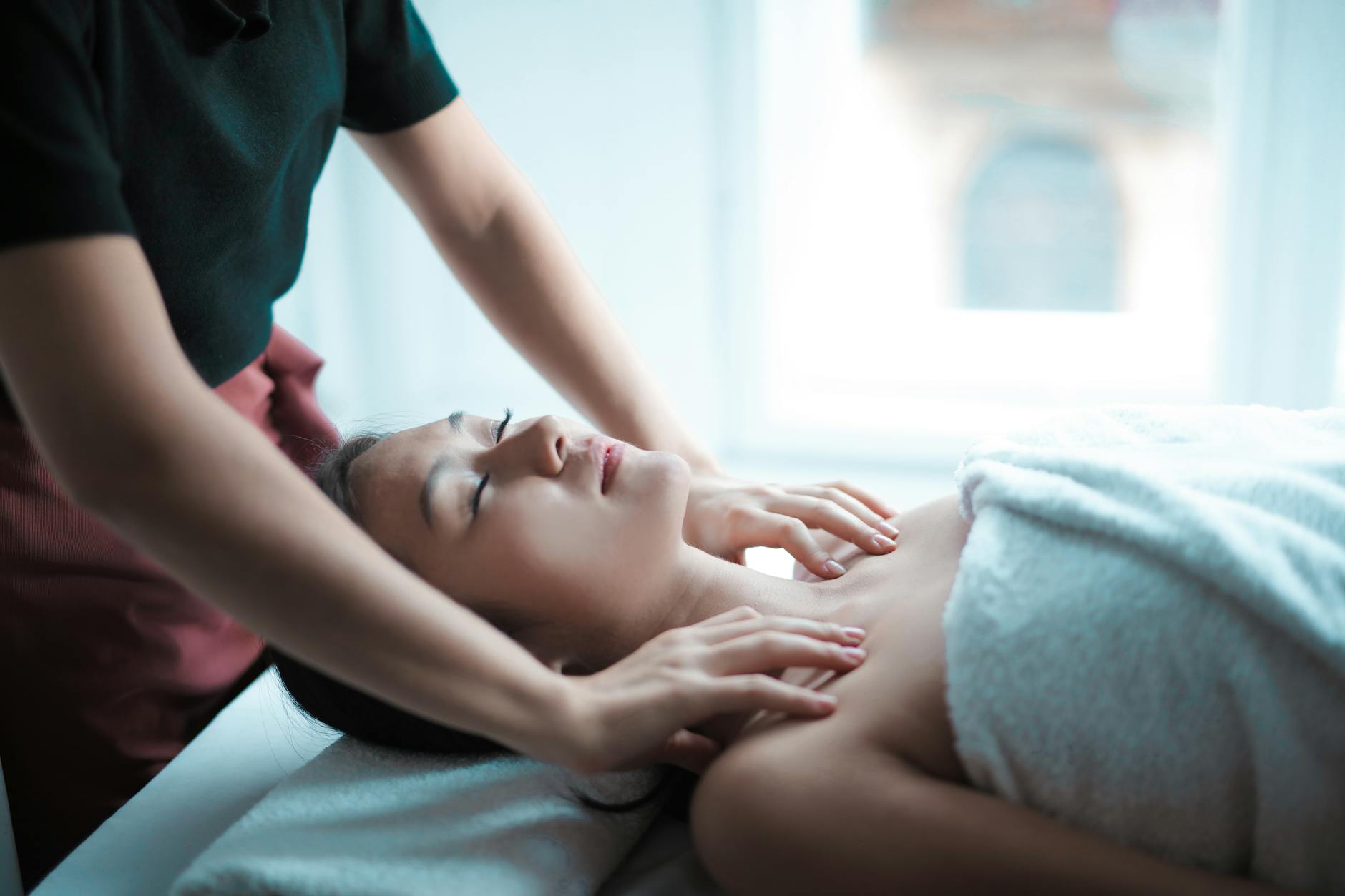
Nurse burnout is one of the most urgent issues in NHS healthcare right now and if you’re working in it, you’re not reading a statistic. You’re living it. The staffing pressures, the back-to-back nights, the emotional weight of what patients and families are going through, and the expectation that you’ll show up for every shift as though none of it accumulates. That is an enormous amount to hold.
Nurse burnout is one of the most urgent issues in NHS healthcare right now and if you’re working in it, you’re not reading a statistic. You’re living it. The staffing pressures, the back-to-back nights, the emotional weight of what patients and families are going through, and the expectation that you’ll show up for every shift as though none of it accumulates. That is an enormous amount to hold.
Here’s what most wellness content gets wrong for shift workers: it assumes you have fixed evenings, predictable days off, and a clinic near you that’s open when you finish work. For nurses on rotating NHS shifts, that assumption makes most self-care advice instantly irrelevant. The recovery options that genuinely work are at-home, on-demand, and bookable around the shifts you actually know you’re working not the ones you hoped you’d have off.
This article covers what nursing burnout actually involves, what’s driving it across the NHS, how it connects to patient safety, and what realistic recovery looks like for someone whose schedule changes week to week.
What Is Nurse Burnout, And How Is It Different From Just Being Exhausted?
Nurse burnout is a state of prolonged physical and emotional depletion that develops when the sustained demands of healthcare work consistently exceed your capacity to recover. The World Health Organisation recognises it as an occupational phenomenon a condition produced by working conditions, not a personal weakness or a failure of commitment.
It shows up in three distinct ways. Emotional exhaustion: the feeling that you’ve given everything and there’s nothing left. Depersonalisation: emotionally withdrawing from patients and colleagues as a psychological coping mechanism when reserves are genuinely depleted. And a reduced sense of personal accomplishment work that once felt meaningful starts to feel mechanical and disconnected.
The important distinction: this is fundamentally different from a difficult run of shifts. Those pass. Burnout is what sets in when they don’t stop when rest no longer restores you, when you start dreading going in rather than feeling ready to.
NHS England’s workforce data reflects a serious picture. A recent NHS Staff Survey found that a significant proportion of nursing staff regularly feel burnt out because of their work, with rates increasing notably since the pandemic. If you recognise yourself here, you are far from alone and the evidence places responsibility squarely with working conditions, not the people doing the work.
Why Are NHS Nurses Burning Out? The Causes That Go Deeper Than One Difficult Week
The causes of nursing burnout are largely structural. Research published in peer-reviewed nursing and health journals consistently identifies the same factors across NHS and international settings:
- Unsafe patient-to-nurse ratios: When the load is too high, every clinical decision carries more risk. The sustained stress of this accumulates in ways that aren’t visible on a rota.
- Irregular and rotating shifts: Night rotations, weekend working, and unpredictable scheduling disrupt sleep quality, circadian health, and social stability in ways that compound over months.
- Emotional labour: Supporting patients and families through acute illness, grief, and fear is deeply demanding work that rarely appears in workload calculations or staffing models.
- Moral distress: Being placed in situations where resource constraints prevent the standard of care you trained for creates a form of occupational injury specific to healthcare.
- Lack of professional autonomy: Feeling unable to influence your working environment or clinical decisions is a consistent predictor of burnout across all healthcare settings.
- Insufficient recognition: When expertise and sustained effort go unacknowledged, the intrinsic motivation that sustains care work erodes.
- Poor workplace culture: Hierarchical dynamics, weak leadership, and interpersonal conflict accelerate exhaustion and reduce psychological safety across entire wards.
Understanding these as systemic causes not individual failings, matters. It shifts the question from “what should nurses do differently” to “what does the system need to change,” while also making clear that individual recovery strategies are still worth pursuing.
Does Burnout Affect the Care You Give Your Patients? Here’s What Research Shows
This is where nursing burnout moves from a workforce welfare concern to a patient safety issue and the evidence is well established.
Studies have linked burnout in clinical nurses to higher rates of medication errors, reduced vigilance for patient deterioration, lower patient satisfaction scores, and poorer infection control outcomes. When you’re operating in chronic depletion, the cognitive and emotional resources required for safe, attentive practice are genuinely reduced.
Within the NHS specifically, the connection between staff wellbeing and patient outcomes is well documented. NHS England’s own research consistently shows that good staff wellbeing correlates with stronger performance across quality and safety indicators and the inverse holds equally.
Burnout also drives attrition. Experienced nurses leaving clinical roles to agency work, management, or leaving the profession entirely places greater burden on remaining staff, accelerating further burnout across the team. Understanding this isn’t about increasing your guilt. It’s about making one point clearly: your recovery matters not as a nice-to-have, but as a direct investment in the care you’re there to provide.
What Does Self-Care Actually Look Like When You Work NHS Shift Patterns?
Standard wellness advice was written for standard schedules. Finishing at 07:30, mid-run of nights, or about to start a stretch of lates? Most of it doesn’t translate.
Here’s what genuinely can:
- Micro-recovery in the gaps: Even 15 to 20 minutes of intentional rest between shifts not phone time, not life admin engages the parasympathetic nervous system and supports faster physical recovery. Short breathwork exercises take five minutes and work anywhere.
- Nutrition planning on rest days: Preparing portable, protein-dense food on your days off removes decisions from the post-shift window, when your brain has nothing left for them. Batch cooking is unglamorous and genuinely effective.
- Home-based movement: Walks, bodyweight exercises, and stretching at home require no gym membership, no commute, and no fixed time slot. Consistency at a manageable level beats intensity that requires more than you have to give.
- Sleep environment investment: Blackout blinds, a cool room, a consistent pre-sleep sequence, and phone-free wind-down time matter significantly for anyone whose sleep timing is irregular. Your environment can do a lot of the work.
- At-home physical recovery: Booking a vetted, insured professional to come to your home removes every barrier that makes clinic-based recovery unrealistic after a long shift. No driving. No waiting rooms. No booking a slot you can’t guarantee you’ll make.
- Deliberate peer time: Scheduled time with colleagues or close friends who understand healthcare provides emotional processing that solo self-care can’t replicate. Put it in the diary like any other commitment.
Forward managers and team leads exploring ways to invest in staff wellbeing across a whole team, at-home and flexible formats are particularly well suited to the access challenges of NHS shift work.
Why Booking a Clinic Doesn’t Work for Shift Workers And What Does
The design of most wellness services creates a specific problem for shift workers that’s rarely acknowledged directly. It isn’t just that clinics close at 6pm it’s the advance booking problem. When your NHS rota changes weekly, you often can’t commit to a 6pm Wednesday appointment you booked a fortnight ago because your schedule might not have been confirmed until three days prior. The model that requires forward planning simply doesn’t fit the reality of how shift rosters work.
Providers you book through Blys can be booked same-day or next-day. That means you can schedule recovery once you actually know your shifts, not before a rota that hasn’t been released yet. It’s a fundamentally different model, and for nurses on rotating patterns, it’s the only one that genuinely works in practice rather than in theory.
Through Blys, you can access vetted, insured professional massage therapists, sports therapists, physiotherapists, and other trusted practitioners who come to your home at a time you specify. You recover on your own terms, in your own space, without adding commuting time to a shift that already ran long.
Planning a wellness break before a demanding stretch is one of the most proactive things you can do to protect your physical and mental reserves before they’re depleted rather than after.
Take Care Of Yourself So You Can Keep Caring For Others
Nursing burnout is a real occupational health issue not a character failing, and not something that improves through persistence alone. The systemic changes required across the NHS take time and sustained advocacy. In the meantime, building recovery into your actual schedule not an ideal version of it is one of the most effective things you can do for your patients, your team, and your own longevity in a profession that genuinely needs experienced people.
Explore what at-home wellness support looks like near you through Blys and find what fits your current roster.